Osteoporosis
Overview: What is osteoporosis?
Osteoporosis, which means porous bones, is a progressive condition in which bones become structurally weak and are more likely to fracture or break. It is sometimes called a “silent” disease, because bone loss often occurs without your knowing it.
Normally, the body forms enough new bone tissue to balance the amount of bone tissue broken down and absorbed by the body. This is a natural process called bone turnover. Throughout the early part of your life, the amount of bone lost and the amount gained remains balanced. Bone mass (size and thickness) increases during childhood and early adult life, reaching its maximum by the age of 20 to 25.
Menopause, which usually occurs in a woman’s 40s or 50s, dramatically speeds bone loss. Older men lose bone mass as they age, as well. Osteoporosis develops when your body loses bone faster than it can form new bone. Over time, the imbalance between bone breakdown and formation causes bone mass to decrease, so fractures occur more easily.
Bones in the hip, spine, and wrist are especially prone to fragility fractures—fractures that would not have occurred in a younger person with stronger bones.
Forty percent of women and 25 percent of men over age 50 will have an osteoporosis-related fracture in his or her remaining lifetime.
Osteopenia, or low bone mass, is a more moderate decline in bone density than occurs in osteoporosis. If you have been diagnosed with osteopenia, or even osteoporosis, you can take steps to prevent further bone loss.
You need to exercise and get enough calcium and vitamin D to help keep your bones strong. You also may need to take medications for osteoporosis treatment. Ask your physician what action is right for you. Physicians agree that postmenopausal women and older men with osteoporosis should be medically treated to prevent fractures.
What role do hormones play in bone disease?
Too much or too little of certain hormones in the body can contribute to osteopenia and osteoporosis.
- During and after menopause, the ovaries make much less of the hormone estrogen. Estrogen loss may also occur with surgical removal of the ovaries or because of excessive dieting and exercise. Estrogen helps protect bone.
- Men produce less testosterone (and estrogen—produced in small amounts in males) as they age. Reductions in these hormones may also contribute to bone loss.
- Bone loss can result from the damaging effects of excess cortisol, as occurs in Cushing’s syndrome. Sometimes the adrenal glands produce excess cortisol because of a pituitary gland or other tumor. More commonly, Cushing's syndrome develops as a result of long-term use of corticosteroid medications (steroids) such as prednisone and cortisone, used to treat inflammatory disorders like rheumatoid arthritis or asthma.
- Other hormone imbalances that may increase the risk of osteoporosis include an overactive thyroid gland, diabetes, and hyperprolactinemia, in which the pituitary gland produces too much of the hormone prolactin.
- Thyroid cancer survivors whose treatment includes high doses of thyroid hormone also have a higher risk.
- Eating disorders, especially anorexia nervosa, increase the risk of osteoporosis. Bone loss occurs partly because of poor nutrition and, in women, partly because the ovaries stop functioning normally, producing less estrogen.
Who is at risk for osteoporosis?
Excessive bone loss occurs more often in certain groups of people. Your risk of developing osteoporosis is higher if you:
- are older
- have a family history of osteoporosis
- have a thin or small frame
- have completed menopause
- are Caucasian or Asian
- have had a fracture as an adult
- have a parent with hip fracture
Other factors that may increase your risk of bone loss include:
- amenorrhea (missing menstrual periods)
- anorexia nervosa
- an inactive lifestyle
- a diet low in calcium or vitamin D
- low testosterone (hypogonadism)
- smoking
- drinking too much alcohol
- certain medications, including some anti-seizure medications, large doses of thyroid hormone, or steroids
- certain hormonal conditions (described above)
Osteoporosis Signs and Symptoms
While osteoporosis symptoms are few, the first sign of osteoporosis is often a bone fracture. Fractures may trigger serious health problems, including disability and even premature death. Many women and men go through life without knowing they have lost bone mass until they break their hip, spine, or wrist and experience the consequences of this otherwise silent disease.
Some people have spine fractures that lead to a curve in their upper back, sometimes called a dowager's hump. The first suggestion of spinal fractures and one of the first symptoms of osteoporosis may be when you realize you are not as tall as you used to be. Other signs and symptoms are back pain and stooped posture. If you have lost more than one inch from your (accurately measured) height as a young adult, you may wish to speak with your doctor about testing for osteoporosis.
More serious problems may occur after a hip fracture, because some people lose the ability to walk normally, perform activities of daily living, or live independently.
If you are a man or woman at risk for bone loss — and especially if you have experienced a fracture after age 50 — you should have a bone mineral density test to monitor the mass of your bones. Ask your doctor about a dual-energy X-ray absorptiometry (DEXA) scan or quantitative low dose CT scan. These safe, simple, and non-invasive tests takes only a few minutes and measures the amount of bone present in the spine and hips, which helps diagnose osteoporosis or osteopenia.
It is recommended that all women aged 65 and older, and men aged 70 or older, should have a bone density test. It is also recommended that younger postmenopausal women and men aged 50 to 69 with risk factors for osteoporosis should be tested.
Others who need to be tested include the following:
- Adults with a condition, such as rheumatoid arthritis, or taking a medication, such as corticosteriods, that may contribute to bone loss
- Anyone whose doctor is considering prescribing osteoporosis drug therapy
Postmenopausal women who are discontinuing estrogen therapy
Osteoporosis Treatment Options
The key to good osteoporosis care is understanding the causes of osteoporosis and knowing the risks of bone fractures. Having a DEXA bone mineral density test reveals important information on your risk for osteoporotic fractures (see Osteoporosis Signs and Symptoms).
Osteoporosis prevention and treatment include exercise and the right amount of calcium in your diet. Most adults over age 50 need 1,200 mg daily, although you may need more if you have osteoporosis. Calcium supplements may be necessary if your diet is not providing enough calcium to keep your bones strong. Taking too much calcium, however, may increase the risk of kidney stones. Vitamin D helps your body absorb calcium. Most adults don’t have enough vitamin D in their bodies.
Older men and women probably should take vitamin D supplements. Current recommendations are for 800 to 1,000 IU (International Units) of vitamin D3 per day, although many people require higher doese. Younger men and women may need to take vitamin D supplements, too. Very high doses of vitamin D can cause serious health problems so talk with your physician about how much is right for you.
A well-balanced diet with calcium-rich foods, plus calcium and vitamin D supplements, however, may not be enough to protect bones and prevent osteoporosis in all people. Each individual’s health and family history are different, so the risk profile for breaking bones differs for each person. Some people may need to take medications to treat osteoporosis.
For Women:
These drugs include:
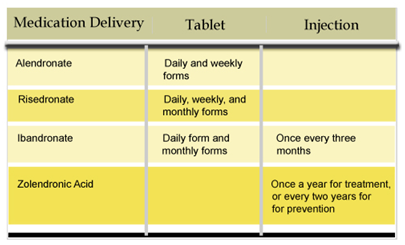
Bisphosphonates: Alendronate, Risedronate, Ibandronate, Zoledronic Acid
Bisphosphonates—which inhibit the breakdown of bone—are used to prevent and treat postmenopausal osteoporosis by slowing bone loss while increasing bone mass. Bisphosphonates help reduce the risk of spine, non-spine, and hip fractures.
Alendronate, risedronate, and zolderonic acid have also been approved for the treatment of steroid-induced osteoporosis in men and women who require long-term use of medications to treat inflammatory conditions (which can contribute to osteoporosis).
If you are taking an oral bisphosphonate, you should take the drug upon arising in the morning after an overnight fast, with one full glass of water. Stay in an upright position after taking the dose.
If you are taking alendronate or risedronate, do not drink or eat anything else for the following 30 minutes so your body can absorb the medication. If you are taking ibandronate, you must wait 60 minutes to eat or drink anything.
Side effects of bisphosphonates are uncommon, but may include abdominal, bone, or muscle pain. These medications may also cause nausea or heartburn. Irritation of the esophagus may occur with the tablet forms of this medication.
Relatively high-dose, long-term bisphosphonate therapy, which might be administered during cancer treatment, for example, has been linked to osteonecrosis (degeneration) of the jaw bone. This problem tends to arise most frequently after dental operations. There is some suggestion that, very rarely, degeneration of the jaw may also develop after relatively low-dose, long-term bisphosphonate treatment by mouth. This is an area of active research investigation. Bisphosphonates are not recommended for pre-menopausal women who may become pregnant.
Calcitonin
Calcitonin is a naturally-occurring hormone made by specialized cells in the thyroid gland. Together with parathyroid hormone, calcitonin helps to regulate calcium levels in the body. Calcitonin, which is given as a nasal spray, has been shown to modestly increase bone density, and may reduce the risk of spine fractures. Its effects on building bone are generally smaller than other approved therapies. Side effects from nasal calcitonin are uncommon, but may include nasal irritation, backache, bloody nose, and headaches.
Selective Estrogen Receptor Modulators (SERMs): Raloxifene
Raloxifene is approved for preventing and treating osteoporosis in postmenopausal women. It is from a class of drugs called selective estrogen receptor modulators (SERMs). These estrogen-like medications were developed to benefit the bone, while avoiding the potential risks associated with estrogen therapy (such as increased risk of breast cancer or heart disease).
Raloxifene increases bone density and reduces the risk of spine fractures, but it has not been shown to decrease the risk of non-spinal fractures. Raloxifene also decreases the risk of invasive breast cancer.
Raloxifene is taken in pill form, once a day, with or without meals. While uncommon, side effects may include hot flushes, leg cramps, or blood clots in the legs or lungs. Raloxifene is not recommended for pre-menopausal women.
Teriparatide
Teriparatide is a fragment or portion of the full-length parathyroid hormone molecule, which is a naturally-occurring hormone involved in calcium regulation. Teriparatide treatment stimulates new bone formation, rather than preventing bone breakdown. Because of potential safety concerns, the use of this drug is restricted to men and women with severe osteoporosis—who have a high risk of a fracture—and can be given for no more than two years.
Teriparatide is given as a daily, self-administered injection. Side effects are uncommon but may include leg cramps, headaches, and dizziness. This medication is not recommended for pre-menopausal women.
Estrogen
Estrogen can be taken alone or in combination with a progestin, a synthetic form of the female hormone progesterone that helps protect against uterine cancer. (If your uterus has been surgically removed, you do not need to take a progestin with the estrogen.)
Estrogen hormone therapy prevents bone loss and reduces the risk of fracture in the spine and hip. It can also relieve other symptoms of menopause, such as hot flushes and vaginal dryness. Estrogen is usually given in pill form, although it is also available in other forms such as a skin patch or gel.
Current consensus is that the risks of estrogen therapy—including heart attack, stroke, blood clots, and breast cancer— need to be considered on an individual basis together with its putative benefits not just on bone density.
For Men:
Alendronate, risedronate, zoledronic acid, and teriparatide have been approved to treat osteoporosis in men. Although there are fewer studies in men, the effects of these agents on bone mass are similar to their effects in women and are likely helpful in treating men with osteoporosis.
The question of whether testosterone supplementation is useful for treatment of osteoporosis in men remains controversial. In men who clearly have low levels of testosterone, treatment with testosterone appears to increase bone density.
Because testosterone levels tend to decline with age, many older men have testosterone levels that are low. Testosterone supplements may improve bone mineral density in these men as well, but the doses necessary and the best way to administer this treatment are unclear. There is no information about whether testosterone treatment in men is effective in reducing fracture risk.
Finally, the risks of long-term testosterone treatment in older men are unknown. At present, it is generally not recommended that testosterone be used as the primary osteoporosis treatment for men. It is important to remember that the approved osteoporosis treatments for men (alendronate, risedronate, zoledronic acid, and teriparatide) seem to be effective in men with low testosterone levels.
Osteoporosis Lifestyle and Prevention
By the year 2020, it is estimated that approximately half of all adults over age 50 will have weak bones unless they make changes in their diets and lifestyles.
The best way to keep your bones healthy is to establish a healthy lifestyle. This is good advice for everyone, of course, but especially true if you have risk factors for osteoporosis. As a start, you can take steps to reduce your risk:
- Stop smoking.
- Reduce alcohol intake.
- Get enough calcium and vitamin D through your diet or with supplements.
- Do weight-bearing exercises to help keep bones strong.
- Avoid high doses of thyroid hormone or cortisone-like medications. If you must take them, work with your doctor to get the lowest possible dose to treat your condition.
Diet and Exercise Make a Difference
Calcium
Diet makes a difference in the prevention of osteoporosis. Calcium, the main element needed to keep your bones strong and healthy, is found mainly in dairy products.
On average, people get 500 mg to 600 mg of calcium in their diet, largely from dairy products. Unfortunately, that is not enough to meet our needs. To get the calcium that you need to keep your bones healthy, you should eat three to four servings of dairy foods daily. Great calcium sources include milk, yogurt, and cheese. Other sources of calcium include some green vegetables such as broccoli and kale.
If you cannot get all the calcium you need from food alone, you may need to take calcium supplements. Likewise, if you are lactose intolerant or limit dairy foods in your diet for other reasons, you can supplement your diet with calcium tablets.
Vitamin D
To form and maintain strong bones, vitamin D is essential. Vitamin D helps maintain a normal level of calcium in the blood by helping the body absorb calcium properly, and has other health benefits as well. Low levels are linked to an increased risk of many diseases including heart disease, diabetes, cancer and low mood. Fortified milk, egg yolks, liver, saltwater fish, and fish oils are among the few foods that contain vitamin D.
Sunlight on your skin activates the production of vitamin D in your body, but many people do not get enough sun to make sufficient vitamin D. While most people need at least 1,000 IU of vitamin D each day, many men and women need even higher doses. You may want to have your doctor do a blood test to see if you are getting enough vitamin D and advise you on how to increase your intake if necessary.
Exercise
Exercise is the other important key to keeping your bones healthy. Exercise improves strength and balance, which may decrease the risk of falling. Before beginning any new physical activities, however, check with your doctor. A 55-year-old woman who is healthy would probably not have trouble beginning a weight-bearing regimen, but a 90-year-old woman might get a fracture doing the same type of exercise, because her bones are not as strong.
Once you get your doctor's okay, try walking more and climbing stairs, or jogging and playing racquet sports. Weight-bearing and strength-training exercise can help you stay fit and may lower the risk of fractures. Even men and women in their 90s have benefited from a gradual, personalized weight-training program. Bones remain stronger if they are used in daily weight-bearing activities such as walking or lifting weights. Walking at least 20 minutes a day can reduce bone loss.
Safety Precautions
Preventing fractures is important at any age. Here is a checklist to keep you safe at home:
- Floors — Remove all loose wires, cords, and small rugs. Make sure your rugs are smooth and anchored. Keep furniture in its place so you won’t bump into or trip over it.
- Bathrooms — Install non-skid tape in the tub and shower, and install grab bars.
- Kitchen — Install non-skid mats near sink and stove. Clean spills right away.
- Stairs — Do not leave piles of clothing or other items on your stairs. Make sure the hand rails and carpeting are secure.
- Lighting — Install good lighting in your halls, stairways, and entrances. Install night lights in your bathroom. Turn on your lights if you have to get up during the night.
- In general — Ask your doctor if any of your medications might make you dizzy or more likely to fall. If you drink alcohol, drink only in moderation. If you feel unsteady, wear only flat, rubber-soled shoes.
Bone loss is a natural part of aging, but there are steps you can take to stay strong during every stage of your life. A healthy lifestyle is a great place to start.
